6 months after Canada’s 1st COVID-19 case, hospitals ‘better prepared’ to help sickest patients

By late March, COVID-19 patients had started trickling in to the already-bustling Brampton Civic Hospital.
One of them, a man in his 40s, had previously been healthy. Now, he was hooked up to oxygen, with a respiratory rate of around 40 breaths each minute — more than double the number an adult would normally take.
Critical care physician Dr. Brooks Fallis first met the man during a consultation, amid concerns the patient’s lungs may be failing fast enough to require a transfer into the intensive care unit, or ICU.
“He was sort of the mirror image of me: Otherwise healthy, early 40s,” Fallis recalls. “That really struck home for me, that, wow, this is going to strike everybody.”
For many physicians leading teams in hospital ICUs, those first few months of the pandemic were marked by uncertainty, and tinged with fear.
News stories and photos kept flowing in from hospitals overseas, where clinical teams in virus hotbeds like Italy donned hazmat suits while scores of patients left in body bags. Anecdotes of what treatment strategies worked — and what didn’t — were shared too, including early notions of rapid ventilation as a way to keep COVID-19 patients from suddenly crashing. On top of that, fears spiked that personal protective equipment was quickly running out.
But now, six months after Canada’s first presumptive case, multiple clinicians who spoke to CBC News say their understanding of COVID-19 has evolved.
While the disease itself remains tough to treat, with questions still lingering over how it ravages the body, critical care teams dealing with the sickest patients feel better equipped to save more lives.
“Now that there are fewer unknowns, I think everyone feels better prepared,” says Dr. Bram Rochwerg, a critical care lead at the Juravinski Hospital in Hamilton, Ont.
“There’s less uncertainty around what to do.”
First case identified on Jan. 25
Back on Jan. 25, Ontario announced the country’s first presumptive positive case of COVID-19 — then just known as an illness caused by a novel coronavirus — had been identified in Toronto.
Cases started to tick upwards after that, with roughly 40,000 confirmed cases across the province to date. At certain points in the pandemic, several hundred people were also in hospital ICUs at any given time.
Early on, the advice circulating around the medical community was to intubate those sick patients fast to get them hooked up to a mechanical ventilator — or risk watching their lung function suddenly plummet.
Fallis says the thinking has since changed.
“It’s not that people can completely nosedive,” he explains. “There is a gradual deterioration, and some people can remain for a long time on high levels of oxygen, breathing on their own. Some people never need a ventilator and start to get better.”
COVID-19 does remain deadly for many people who fall seriously ill, often thanks to major inflammation and eventual lung failure that’s known as acute respiratory distress syndrome, or ARDS.
It’s a condition long tied to other infections like severe pneumonia or sepsis, a major infection of the bloodstream.
Dr. Donna McRitchie, an intensive care specialist at North York General hospital and the facility’s vice president of medical and academic affairs, says critical care teams are now shifting to more traditional methods of treating ARDS — not the rapid ventilation approach initially used for COVID-19 patients.
That means less rushing, and more watching and waiting to see how patients fare on oxygen treatments, and on hooking them up to a ventilator only when absolutely necessary.
“In a way,” McRitchie says, “the new standard is the old standard.”
Strategies ‘buying time’ for lungs to heal
For patients whose lung function does drop enough to require mechanical ventilation, many critical care specialists now agree that “proning” — flipping a patient onto their front for stretches of time — can help blood flow and oxygen intake.
Yet again, it’s not a new concept, but one that does seem to benefit COVID-19 patients as well, Fallis says.
In the William Osler Health System, where he’s medical director and division head of critical care, there is now a “proning team” to carry out the labour-intensive flips.
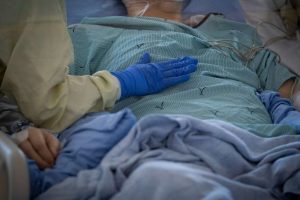
After a patient is intubated and using a ventilator, the team — usually two health-care workers on either side, one at the patient’s feet coordinating, and one at their head making sure the breathing tube stays in place — carefully flip the person onto their front.
The patients spend at least 16 hours a day in that position, with staff turning their head left or right every two hours.
Some COVID-19 patients have an “unbelievable response” to the time-consuming positioning, which Fallis says helps boost their lung function, allowing clinical teams to use more gentle ventilation rather than higher settings that can do more harm than good to inflamed tissue.
“These things don’t make the lungs better,” he clarifies. “It’s buying time for the lungs to get better on their own.”
Steroid use as treatment now common
At the same time, clinicians are now watching closely for other impacts of the illness beyond the lungs, since it’s now clear COVID-19 can wreak havoc on various areas of the body.
McRitchie says some seriously ill patients are experiencing everything from renal failure to constant blood clotting. The difference now is that physicians are actively searching for these “potential complications,” she adds.
“We’ve just never seen anything on this kind of level in our lifetime,” stresses Fallis.
“When your lungs fail, your organ system becomes like a house of cards, where it can all fall apart. The more organ systems fail, the more likely you are to die.”
That’s why so much hope is pinned on a successful treatment for the disease, beyond the interventions provided by critical care teams.

Dr. Rob Fowler, a critical care physician at Sunnybrook Hospital — the facility that treated the country’s first confirmed case — says initially, clinicians really had no sense what, if any, medications would be effective against the disease.
While there’s still no miracle drug to cure COVID-19, the physicians who spoke to CBC News all agreed dexamethasone — a steroid used since the 1960s to reduce inflammation — has been the most successful at reducing mortality rates.
As the World Health Organization noted back in June, the treatment was shown to reduce mortality by about one third for patients on ventilators, and by around one fifth for patients needing only oxygen support, according to preliminary findings from clinical trials in the United Kingdom.
“In a rather short period of time, we’ve gone from not having any idea of whether this was a valid treatment, to knowing this, in fact, would save a lot of lives,” Fowler says.
Hospitals acting as ‘safety net’
Overall, the changes in patient outcomes remain small, Rochwerg says, though clinicians do feel better prepared to treat seriously ill cases — thanks to a combination of tested strategies, and greater confidence in hospital protocols and access to protective gear.
In the case of steroids, which he says are now being used for upwards of 90 per cent of ventilated COVID-19 patients, they are medications that are relatively “simple, cheap, and widely available” compared to other treatments making headlines.
Fallis, whose teams are also giving dexamethasone to nearly all seriously ill COVID-19 patients on oxygen or a ventilator, also warns the disease itself remains just as deadly.
“If a large number of people get it, a large number of people will die,” he stresses. “Even with the best care.”
Looking back on his first experience with a COVID-19 patient in March, Fallis says that man in his 40s wound up not needing a ventilator. After a few days on oxygen, he was well enough to go home.
Those are the success stories physicians want more of — but more challenges lie ahead.
The focus this fall, Fallis says, amid more businesses reopening and students likely returning to school, is to stave off a second wave of cases in the community to make sure as few people as possible wind up in hospitals in the first place.
“We’re here as the safety net for cases that do slip through,” he adds, “but there’s no way the hospitals can take care of everyone who gets it if it runs wild.”
CBC







Redes Sociais - Comentários